How digital improvements can aid the NHS… Leave a comment
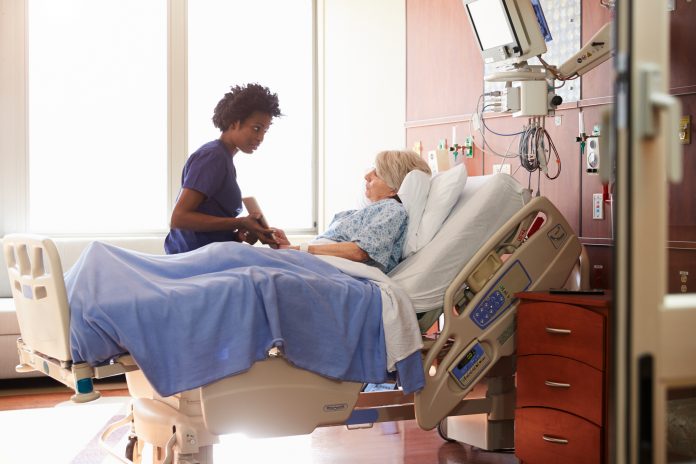
Transforming UK healthcare means tackling the NHS backlog from COVID-19, could this be solved through digital improvements like AI and cloud data?
Since the UK repealed its final COVID-19 laws, many of us have enjoyed a long-awaited, carefree return to relative normality. Unfortunately, the same cannot be said for those using, and working in, healthcare. The NHS backlog, caused by the disruption of normal care by urgent treatment for COVID patients, is still growing in size.
In March 2020, NHS England waiting lists documented 4.24 million patients scheduled for consultant-led elective care. Over two years on, the latest figures show this has risen to 6.63 million—an increase of more than 50%.
The dangers of this backlog are clear. Not only are patients suffering from longer-term pain and poorer health, with some even resorting to costly loans and crowdfunding initiatives to pay for private treatment, but increased workloads mean doctors themselves are reporting the highest levels of professional burnout since records began. So, how can we improve these issues? Carolina Wosiack, Managing Director EMEA, CI&T explores this through key changes to be made in UK healthcare.
Implementing changes to the NHS
As in all walks of life, it’s important to use lessons learned from a negative experience to make impactful, lasting improvements. Here, insights gleaned from the pandemic can be used to transform how we look at healthcare. Just as war drives technological advancement, so too do medical crises: alongside the record-shattering speeds of vaccine development, modern technologies such as AI and cloud data storage are now being crafted to enhance the care that doctors, nurses, and hospitals provide.
The pandemic also highlighted areas for improvement that can’t be solved by innovation alone. To create healthcare services fit for the future, professionals must leverage a combination of new technological, managerial, and administrative solutions to safely prepare for whatever the world throws at us next.
1. Harness innovation for faster, more effective healthcare
Though technology in its current state can never replace the care offered by a healthcare professional, it can help safely tide over the gaps between diagnosis and treatment. Take mental health, for instance.
In England, around 1.6 million people currently sit on the NHS waiting list for mental health care, while 8 million more cannot access specialist help because their mental health problems are not considered serious enough to qualify. Fortunately, AI-powered therapy chatbots such as Wysa are now being trialled on the NHS, in the hope they can maintain and even improve symptoms while patients wait for care. While technology is often seen as a cause of poor mental health, here it can form part of the solution.
Meanwhile, artificial intelligence can even help to reduce wait times and ease pressure on practitioners, too. Tools such as Symptoma claim a +95% diagnosis accuracy rate for over 20,000 diseases and can be used as the first port of call to screen patient’s symptoms and direct them towards precise care for a faster, more effective journey—while freeing up healthcare professionals to focus on other pressing tasks. And then there’s hardware, too.
New wearable technologies, like portable ECG and blood pressure monitors, offer clinicians fresh opportunities to check patient progress remotely. Wearables such as Fitbits help users to stay fit and healthy with activity reminders and even pinpoint when treatment is needed through alerts such as low blood oxygen levels. Meanwhile, new home-based devices, such as home haemodialysis machines, allow patients to undergo dialysis from the comfort of their own homes while freeing up hospital beds for urgent inpatients. With such indisputable benefits, it’s time we embrace technology at every stage of care.
 © Martinmark
© Martinmark
2. Bridge gaps between patient and provider
Early in the pandemic, usage of telehealth services surged as clinicians attempted to deliver safe, effective healthcare from remote, socially-distanced locations. Ever since, the adoption of telehealth has continued to climb, particularly in fields such as radiology, cardiology, and behavioural health, with analysts predicting it to become a $636bn industry by 2028.
To improve on-site waiting times and treat patients who struggle to travel, UK healthcare providers should continue to communicate and diagnose patients over the phone or via video calls where appropriate. The Scottish government’s Near Me programme is a prime example of the potential success of flexibility—by using the Attend Anywhere platform to offer remote healthcare, uptake has grown from 7,000 consultations in 2019 to over a million annually in a handful of years. Plus, 75.1% of Near Me patients and 87.9% of clinicians agreed it will remain a valuable service even now social distancing is no longer required, citing benefits like faster access to support, greater convenience, lower wait times, and reduced environmental impact.
Yet in the UK, there’s still scope for innovations such as telehealth to be implemented further. Healthcare providers must be curious and receptive, pausing any preconceived or traditional ideas to explore the perks of these new, advanced healthcare ideas. Meanwhile, tech developers should work to bridge the knowledge gap between their services and clinicians through training and support to ensure even wider, more effective uptake.
3. Rebuild a system fit for 2022 and beyond
However, the key to many of these improvements is a redevelopment of the NHS system. Currently, the system is designed to provide healthcare to the whole population, not treat individuals, each with specialised needs. Most NHS England patients don’t even own their personal data—even though evolving trends now mean more people want access to make their own decisions. So, this post-pandemic period is a perfect opportunity to rethink the NHS and how it delivers care.
This isn’t simply a case of upgrading the NHS smartphone app to offer more features (although it’d be a good start). A genuine improvement would require the creation of a digital ecosystem and destination, to which patients, nurses, doctors, and hospitals can all connect and communicate through. Then, self-service features would allow patients to easily book appointments, use instant messaging to access healthcare advice fast, and much more. These features would also remove unnecessary time-consuming admin, such as waiting for an appointment letter to arrive, to ensure both individual and nationwide care is prompt and effective.
In addition, the government needs to reintroduce task forces, such as the National Quality Improvement Taskforce for children and young people’s mental health, which previously analysed in-depth how to enhance nationwide healthcare processes. These taskforces can harness expertise from cross-departmental members to ensure specialist study, collaboration, and resolutions for the nation’s toughest healthcare challenges.
Then, data-backed recommendations can be made and implemented for rapid system evolution. And though other priorities such as the cost-of-living crisis currently dominate the headlines, the taskforces must begin their work sooner rather than later. After all, now that we’re over the worst of COVID-19, the time to prepare for the next healthcare crisis is today.